A Complete Guide to Essential Hospital Equipment and Their Functions
Hospital equipment forms the backbone of modern healthcare delivery, enabling medical professionals to diagnose, treat, and monitor patients effectively. From basic diagnostic tools to advanced life-support systems, each piece of equipment serves a critical role in patient care. Understanding these essential devices, their functions, and their importance helps healthcare facilities maintain high standards of care while adapting to evolving medical needs and regulatory requirements.
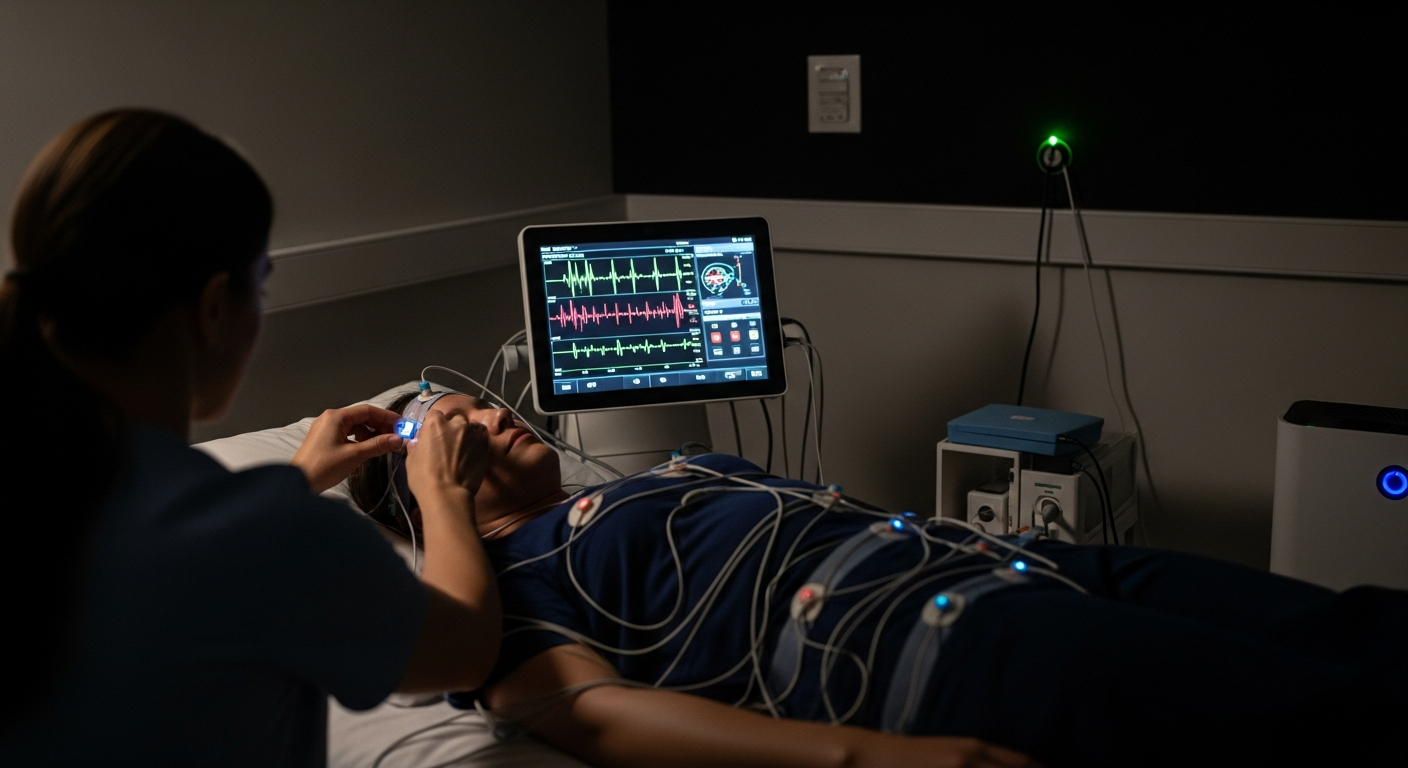
Modern healthcare facilities rely on a diverse range of equipment to provide comprehensive patient care. These tools enable accurate diagnosis, effective treatment, and continuous monitoring of patient conditions. As medical technology advances, hospitals must balance traditional equipment with innovative solutions while ensuring compliance with safety standards and regulatory frameworks.
Why Essential Hospital Equipment Matters Today
The quality and availability of hospital equipment directly impact patient outcomes and healthcare delivery. Diagnostic equipment such as X-ray machines, CT scanners, and ultrasound devices allow physicians to identify medical conditions quickly and accurately. Treatment equipment including surgical instruments, infusion pumps, and ventilators enable medical teams to perform procedures and manage critical conditions effectively. Monitoring devices like electrocardiograms, pulse oximeters, and blood pressure monitors provide real-time data that guides clinical decisions.
Patient safety depends heavily on properly functioning equipment. Defibrillators can restore normal heart rhythm during cardiac emergencies, while anesthesia machines ensure safe sedation during surgical procedures. Laboratory equipment enables accurate testing of blood samples, tissue specimens, and other biological materials, forming the foundation for evidence-based treatment plans. Sterilization equipment prevents infection transmission by ensuring surgical instruments and medical devices meet stringent hygiene standards.
Accessibility to essential equipment affects healthcare equity across different regions and facilities. Well-equipped hospitals can handle complex cases and emergencies, while facilities lacking critical equipment may need to transfer patients elsewhere. This reality underscores the importance of strategic equipment planning and investment in healthcare infrastructure.
Trends and Developments in Hospital Equipment
Technological innovation continues reshaping hospital equipment capabilities. Digital imaging systems now offer higher resolution and faster processing than traditional film-based methods, reducing radiation exposure while improving diagnostic accuracy. Portable ultrasound devices bring imaging capabilities to patient bedsides, emergency rooms, and remote locations, expanding access to diagnostic services.
Minimally invasive surgical equipment has transformed many procedures that once required large incisions and extended recovery periods. Laparoscopic instruments, robotic surgical systems, and endoscopic tools allow surgeons to perform complex operations through small openings, reducing patient trauma and hospitalization time. These advances require specialized training but offer significant benefits for patient comfort and outcomes.
Connectivity and data integration represent major trends in hospital equipment development. Modern devices increasingly connect to electronic health record systems, automatically documenting vital signs, test results, and treatment parameters. This integration reduces manual data entry errors while providing healthcare teams with comprehensive, real-time patient information. Remote monitoring capabilities allow specialists to review patient data and equipment performance from different locations, supporting telemedicine initiatives and expert consultations.
Artificial intelligence and machine learning are being incorporated into diagnostic equipment to assist with image interpretation, pattern recognition, and early disease detection. These technologies complement human expertise rather than replacing it, helping clinicians identify subtle abnormalities and make more informed decisions.
How Regulations Influence Hospital Equipment
Regulatory frameworks govern hospital equipment throughout its lifecycle, from manufacturing and approval to installation and maintenance. Health authorities worldwide establish standards that medical devices must meet before entering clinical use. These regulations address safety, effectiveness, quality control, and performance specifications, protecting patients from substandard or dangerous equipment.
Manufacturers must demonstrate that their equipment meets regulatory requirements through rigorous testing and documentation. Clinical trials may be required for novel devices, while established equipment categories follow standardized approval pathways. Regulatory agencies review technical specifications, manufacturing processes, and risk management systems before granting market authorization.
Healthcare facilities face ongoing compliance obligations related to equipment use and maintenance. Regular calibration ensures measurement accuracy for diagnostic and monitoring devices. Preventive maintenance programs identify potential problems before equipment failures occur, reducing downtime and safety risks. Documentation requirements mandate detailed records of equipment inspections, repairs, and performance verification.
Staff training represents another regulatory consideration. Healthcare workers must demonstrate competency in operating complex equipment safely and effectively. Manufacturers typically provide initial training, while facilities maintain ongoing education programs to address updates, new features, and best practices. Proper training reduces user errors that could compromise patient safety or equipment performance.
Regulations also address equipment disposal and environmental considerations. Medical devices may contain hazardous materials requiring special handling during decommissioning. Electronic waste regulations govern the recycling and disposal of outdated equipment, promoting environmental responsibility within healthcare operations.
Quality management systems integrate regulatory requirements into daily operations. Hospitals establish protocols for equipment selection, procurement, installation, and monitoring that align with applicable standards. Internal audits verify compliance, while external inspections by regulatory authorities ensure facilities maintain required standards. Non-compliance can result in penalties, operational restrictions, or loss of accreditation.
The regulatory landscape continues evolving as technology advances and new safety concerns emerge. Healthcare facilities must stay informed about changing requirements and adapt their equipment management practices accordingly. This dynamic environment requires ongoing attention to regulatory updates, industry guidance, and best practices that support safe, effective patient care.
Conclusion
Essential hospital equipment encompasses a broad spectrum of devices that enable modern healthcare delivery. From diagnostic imaging and laboratory analysis to surgical intervention and patient monitoring, each category of equipment plays a vital role in clinical practice. Understanding equipment functions, staying current with technological developments, and maintaining regulatory compliance ensures healthcare facilities can provide high-quality care while adapting to evolving medical needs and standards.




