The Mechanics of Screwless Dental Implants: Structural Innovations in Restoration
Screwless implant restoration depends on precise engineering rather than a visible fastening bolt. Tapered interfaces, controlled friction, and surface design work together to stabilise components, limit micromovement, and support bone healing when the case and technique are suitable.
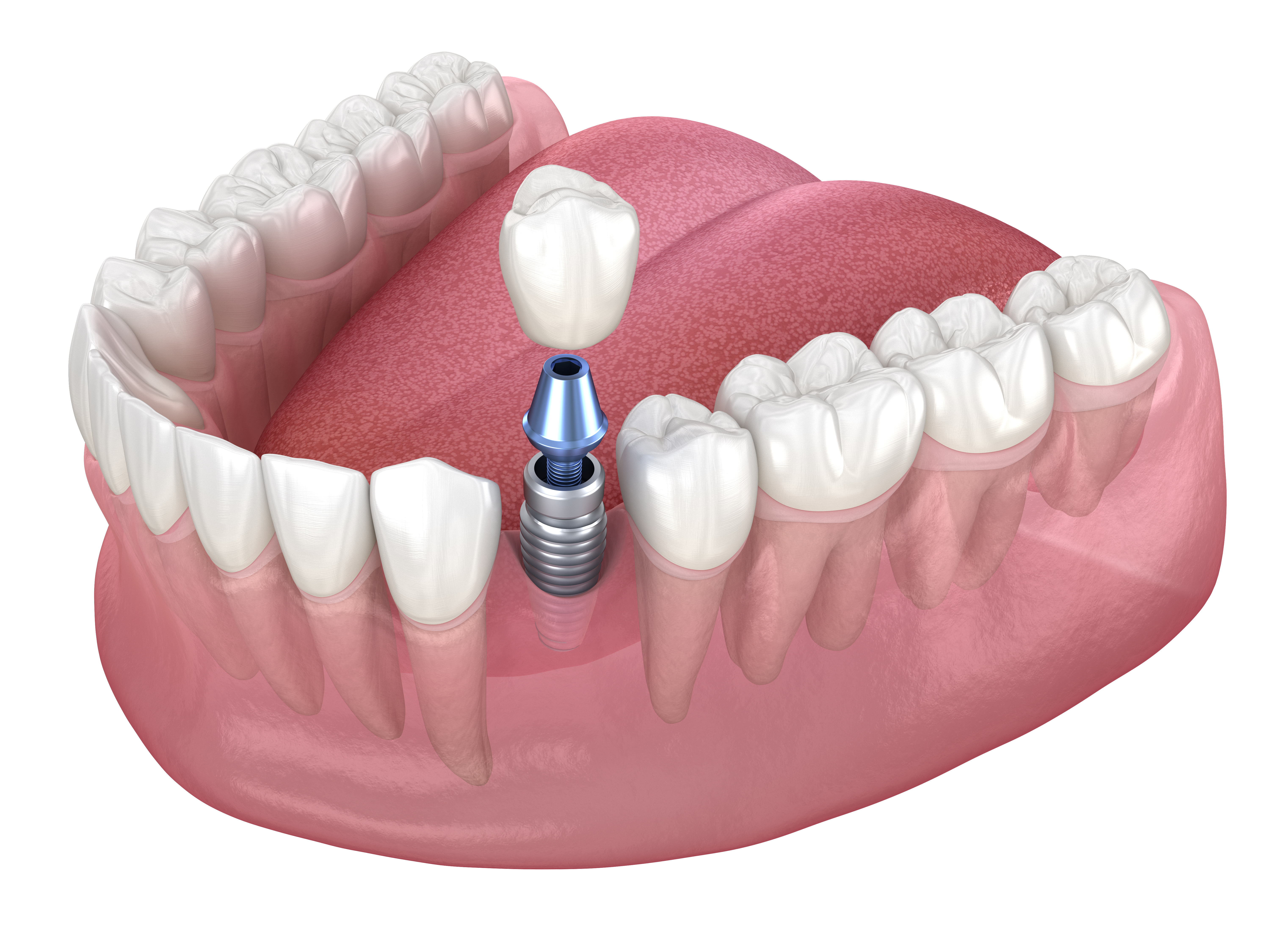
In restorative dentistry, so-called screwless implant designs focus on how parts lock together at a microscopic and mechanical level. Instead of relying primarily on a prosthetic screw to hold the visible restoration in place, these systems often use tapered internal connections, friction-generated retention, and carefully machined contact surfaces. For Australian patients and clinicians, the appeal lies in structural stability, reduced microgaps, and cleaner restorative contours, although success still depends on case selection, surgical planning, and long-term maintenance.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.
How Does Friction-Fit Hold a Prosthetic?
A friction-fit mechanism works by bringing two highly precise components together so that their contact creates resistance to separation. In implant systems, this is commonly achieved through a conical or locking-taper connection between the implant body and the abutment. As the parts seat, the taper generates compressive forces along the interface, which helps limit rotation and movement. In practical terms, that means the restoration can remain stable without depending on an external bolt at that exact junction. This approach also aims to reduce the tiny spaces where bacteria and fluid may collect, although no connection is completely immune to wear, contamination, or loading errors.
The engineering challenge is tolerance control. A friction-fit interface only performs well if manufacturing is consistent at a very fine scale. If the taper angle, surface finish, or seating force varies too much, retention may be weaker than intended or component retrieval may become unnecessarily difficult. That is why screwless concepts are not simply a matter of removing a screw; they are a redesign of the connection itself, with emphasis on fit, preload distribution, and resistance to bending forces created during chewing.
What Changes in Press-Fit Design?
Press-fit technology differs structurally from traditional screw-retained arrangements because the joint is designed to behave more like a wedged interface than a clamped stack of parts. In a classic screw-retained restoration, tightening torque creates preload and holds the assembly together. In a press-fit or locking-taper design, geometry becomes the main retention tool. The deeper and more precise the taper, the more the system can resist micromovement under functional load. Many designs also combine platform switching, internal conical walls, or deeper engagement zones to improve force distribution into the implant and surrounding bone.
Different commercial systems illustrate how manufacturers apply these structural ideas in distinct ways. Not all of the examples below are fully screwless in every restorative step, but they show the range of connection strategies used in contemporary implant design.
| Product/Service Name | Provider | Key Features |
|---|---|---|
| Bicon Implant System | Bicon | Locking-taper connection, screwless implant-abutment retention, plateau-style implant body |
| Ankylos C/X | Dentsply Sirona | Deep conical connection, platform-switching concept, emphasis on connection stability |
| Straumann Bone Level Tapered | Straumann | Tapered body, internal connection design, intended to support primary stability |
| NobelReplace Conical Connection | Nobel Biocare | Internal conical connection, restorative flexibility, focus on stable component seating |
These examples matter because connection geometry affects more than retention alone. It also influences how forces are transferred to the crestal bone, how easily the prosthesis can be retrieved, and how soft tissue contours are managed around the emergence profile. In Australia, the exact systems used in practice vary by clinician training, laboratory workflow, component availability, and regulatory pathway, so the structural concept is often more important than the brand name when comparing treatment designs.
How Do Bioactive Surfaces Aid Integration?
Mechanical stability is only part of the restoration story. The implant surface itself plays a major role in how quickly and predictably bone attaches to the fixture after placement. Bioactive or bioresponsive surfaces are engineered to encourage protein adsorption, cellular attachment, and early bone formation at the interface. This may involve controlled roughness, chemical modification, hydrophilic treatment, or coatings intended to improve the biological environment during early healing. When primary stability from the implant design is paired with a surface that supports osseointegration, the overall system may better resist the transition from surgical placement to functional loading.
That said, a bioactive surface does not override basic biomechanics. Bone quality, implant position, occlusal loading, gum health, and patient-specific healing factors remain decisive. A surface can support integration, but it cannot compensate for poor three-dimensional placement or uncontrolled bite forces. For that reason, modern restoration design is increasingly viewed as a combination of three interlocking elements: the macro shape of the implant, the micro precision of the connection, and the biological behaviour of the surface. Screwless concepts fit into this broader framework because they try to create a more unified implant-abutment-restoration complex rather than a structure dependent on one central fastening point.
Seen from an engineering perspective, screwless implant restoration is less about removing hardware and more about shifting where stability comes from. Friction-fit and press-fit designs aim to secure components through geometry, precision, and controlled contact, while bioactive surfaces support the biological side of fixation in bone. The result is a restorative approach that can offer clean prosthetic design and strong structural performance when used appropriately. Even so, long-term outcomes still depend on diagnosis, clinician technique, maintenance, and the specific implant system chosen for the individual case.




