The Mechanics of Screwless Dental Implants: Structural Innovations in Restoration
Screwless, or screw-retained alternatives, aim to stabilize a tooth replacement using engineered friction, precise geometry, and surface science rather than a visible fastening screw. Understanding how these systems lock together can help patients and clinicians discuss fit, maintenance, and long-term stability in a more informed way.
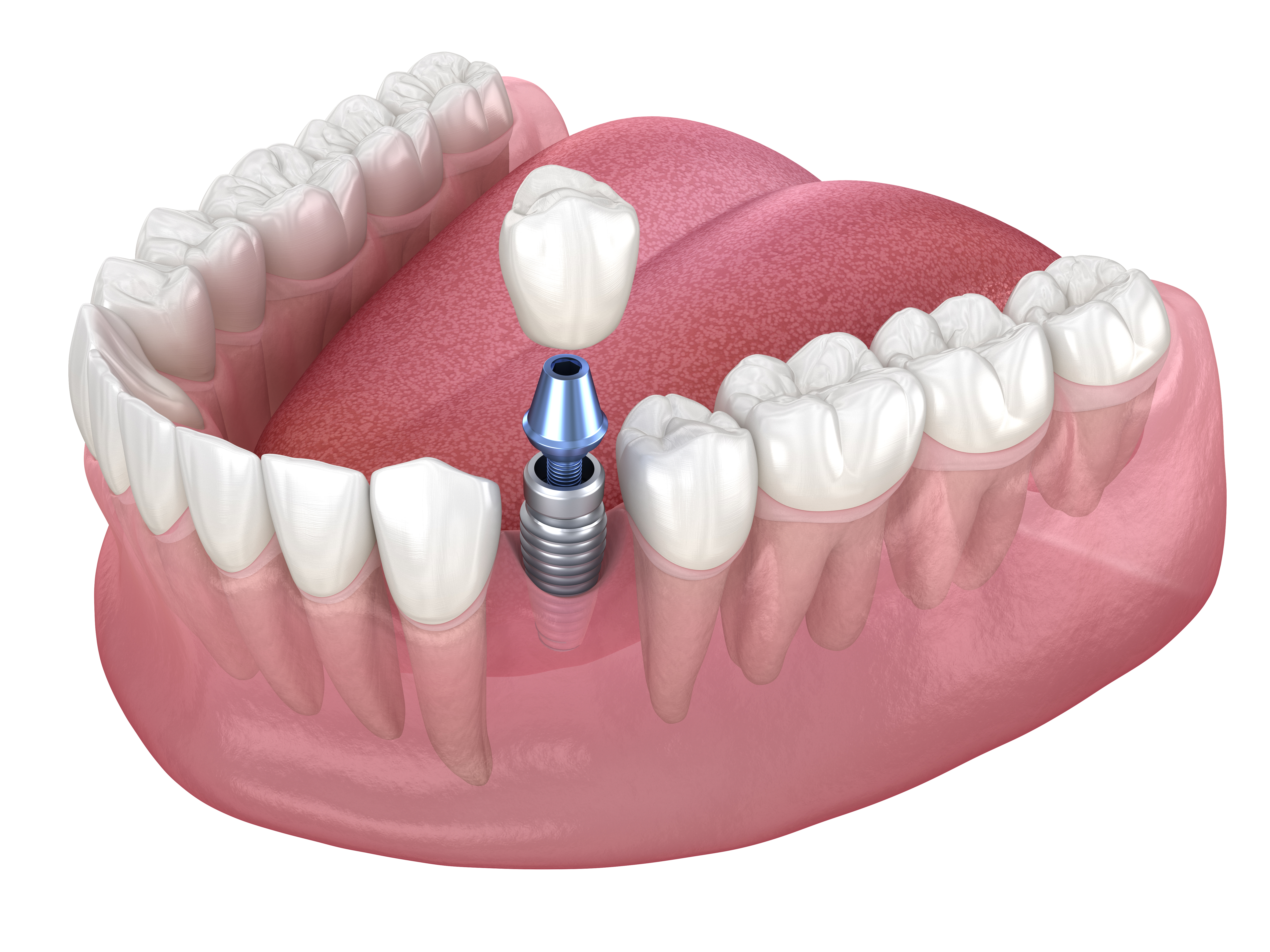
A growing number of modern tooth-replacement systems focus on securing parts through precision fit rather than a traditional retaining screw. These designs rely on controlled friction, taper angles, and carefully matched components to keep a crown or bridge stable under everyday biting forces. They are often discussed in the context of simplifying maintenance and improving aesthetics.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.
How Friction-Fit Mechanisms Secure the Prosthetic Without Mechanical Bolts
Friction-fit retention typically uses a tapered connection, often described as a conical or Morse-taper style interface, where two components wedge together as they seat. The stability comes from intimate contact across a large surface area, which increases resistance to pull-out and micromovement. In practical terms, that means the restoration is held by geometry and frictional forces instead of a separate fastener.
A key idea is that the connection is engineered to distribute load evenly. When biting forces travel through the crown and into the supporting structure, a well-designed taper can reduce the concentration of stress at a single point. This can be relevant for long-term mechanical integrity, because repeated micro-movements can contribute to wear, loosening, or complications at the interface.
In clinic workflows, friction-fit designs may change how retrieval and servicing are approached. Some systems are intended to be retrievable with specialized tools and controlled force, while others behave more like a semi-permanent lock. For patients, the takeaway is that screwless does not mean maintenance-free: cleaning access, bite adjustment, and periodic checks still matter, especially if there is bruxism (teeth grinding) or a complex bite.
Evaluating the Structural Differences in Press-Fit Technology
Press-fit approaches are often associated with the way components seat through tight tolerances, sometimes with elastic deformation at microscopic levels. While the exact engineering varies by manufacturer, the general goal is the same: create a stable joint that resists rotation and vertical displacement without relying on a screw channel through the biting surface.
One structural difference is how anti-rotation features are handled. Screw-retained designs commonly use indexed geometries plus the clamping force of a screw. In press-fit or taper-dominant designs, the anti-rotation effect may come from internal flats, lobes, or polygonal indexing combined with the frictional lock. This can influence how sensitive the system is to component mismatch, wear, or small inaccuracies during seating.
Another difference is how the design manages microgaps. Any tiny gap between components can become a pathway for fluids and bacteria, which is why precision manufacturing and correct seating protocols are emphasized. From a patient perspective in Canada, it is worth asking a local services provider how they verify fit (for example, radiographic checks, torque protocols when applicable, and occlusal adjustment) and how they plan follow-up to monitor the surrounding soft tissue and bone.
The Role of Bioactive Surfaces in Accelerating Bone Integration
Surface technology is a major reason modern systems can perform predictably in a wide range of cases. Many devices use micro-roughened or chemically modified surfaces to encourage bone cells to attach and remodel around the fixture. Some surfaces are described as bioactive when they are designed to interact more directly with the biological environment, potentially supporting faster early stability.
It helps to separate the marketing language from what matters clinically: surface characteristics can influence early healing dynamics, but they do not replace fundamentals such as adequate bone volume, good surgical technique, and patient-specific risk management. Factors like smoking, uncontrolled diabetes, certain medications, and oral hygiene can still affect healing and long-term outcomes.
In real-world planning, surface choice is only one part of the system. The connection type (including friction-fit), the prosthetic design, and the forces from the bite all interact. A well-matched plan considers whether the case needs immediate loading, how many units are being restored, and whether a patient has habits that increase mechanical demand. Discussing these elements with a qualified clinician can clarify why one connection and surface strategy is chosen over another.
Long-term success also depends on maintenance. Even when the fixation is screwless, routine professional monitoring can identify early inflammation, bite wear, or chipping that might otherwise progress. Patients can support outcomes by using interdental cleaning aids appropriate to their restoration design and by attending regular checkups so the fit and surrounding tissues are assessed over time.
Screwless retention concepts highlight how modern restoration design blends mechanical engineering with biology. Friction-fit and press-fit connections aim to improve stability through precision geometry, while advanced surfaces focus on supporting bone response during healing. The most useful way to view these innovations is as tools within a broader treatment plan that still depends on diagnosis, careful placement, and consistent maintenance.




